Novel Optoacoustic Temperature Measurement Technique Enhances Retinal Laser Treatment Safety
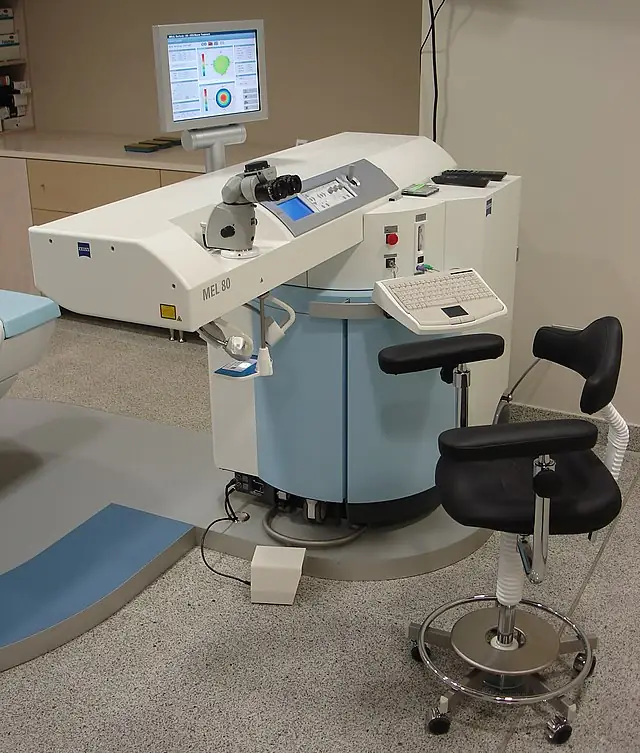
A groundbreaking study has explored a highly accurate and rapid method for measuring temperature during retinal laser treatment with pulse durations of 5µs and longer. This research could pave the way for safer laser treatments tailored to individual patients, considering their specific pigmentation variations. Utilizing an optoacoustic technique, researchers successfully determined the maximum temperature at the end of an irradiation with a single microsecond laser pulse. This new approach could provide medical professionals with a better understanding of the temperature associated with cell damage, potentially minimizing side effects and improving patient outcomes.
While retinal laser treatments like photocoagulation have long been used to repair damaged tissue in the eye, these procedures can cause injury to the retinal pigment epithelium (RPE) and choroid. This likelihood of cell damage varies depending on an individual’s pigmentation, increasing the importance of a tailored approach. Until now, the relationship between temperature and cell damage during laser treatment was not well understood. However, this latest study has showcased how an optoacoustic temperature measurement technique enables accurate assessment of treatment temperatures, shedding light on these factors and supporting safer treatments in the future.
In this innovative investigation, a 15W diode laser with 514nm and variable pulse duration was used to irradiate porcine RPE, a model that closely resembles human RPE. It was found that gradients of the laser pulse flanks >10W/µs excite pressure transients, which in turn enabled optoacoustic temperature measurements. This technologically advanced technique allowed researchers to monitor transient pressure changes during laser irradiation and accurately measure the temperature of the RPE during treatment.
Significantly, the researchers discovered that cell damage occurred at maximum temperatures around 80°C at pulse durations of 35µs to 50µs. This finding could be a game-changer for ophthalmologists, as it provides insight into the precise temperatures at which cell damage is likely. By understanding this critical threshold, medical professionals can better tailor laser treatments to individual patients and minimize the risk of complications post-treatment.
In today’s fast-paced healthcare environment, advancements in technology that equip medical professionals with new tools and techniques are essential for improving patient outcomes. As such, this breakthrough in temperature measurement and its impact on retinal laser treatments could translate into significant benefits for both patients and the broader medical community. For example, a more accurate and rapid temperature measurement method could lead to fewer side effects from retinal laser treatments and a reduced risk of complications, such as scarring and vision loss.
However, as with all new research, there are questions that remain to be answered and areas of further investigation. For one, this study focused on porcine RPE—a close, yet not perfect, approximation for human RPE. While the results may provide valuable insights into the potential risks and outcomes of human retinal laser treatments, further research with human RPE will be necessary to confirm the findings’ applicability to actual clinical scenarios. Additionally, further exploration into the optimal pulse duration and laser energy for different pigmentation levels would help establish a more accurate basis for tailoring treatments.
Despite these limitations, this groundbreaking study represents an immense advancement in the field of retinal laser treatment. By developing a highly accurate and rapid method for measuring temperature during treatment, researchers have brought the medical community one step closer to safer, personalized laser treatments for patients worldwide.
As science enthusiasts, researchers, and students continue this exploration into the relationship between temperature measurement and retinal laser treatment, the potential benefits for policy, public health, and technology cannot be denied. The discovery of a link between temperature and cell damage could serve as a foundation for refining laser treatment protocols, with potential impacts spanning from improved treatment outcomes to cutting-edge medical innovations.
In conclusion, it is essential to acknowledge this research’s vital role in enhancing our understanding of the relationship between temperature and cell damage during retinal laser treatments. As a result, this new optoacoustic technique represents a promising and innovative step towards improving patient outcomes and potentially revolutionizing the field of ophthalmology. With the potential to impact public health, policy, and practice, this novel technique could be a key factor in ensuring the safety and efficacy of retinal laser treatments for generations to come.